This is part of our ongoing series, The Value of Coverage.
Approximately 38 million adults in the U.S. have type 2 diabetes, a costly and often debilitating health condition that occurs when the body cannot properly control blood sugar. About 9 million adults with diabetes are undiagnosed.1 Without proper management, diabetes increases the risk of cardiovascular disease, blindness, kidney failure, and early mortality.
Medical costs associated with diabetes have risen by 35% over the last 10 years, as more people develop the condition and its complications. In 2022, the total cost of treating diabetes in the U.S. was more than $400 billion.2 Employers and the economy bear an additional burden, as diabetes is linked to lost productivity, absenteeism, disability, and early retirement.3 Early detection, proactive care, and appropriate medication are critical strategies for reducing costs and improving long-term health outcomes.4
An additional 98 million adults have prediabetes, a condition in which blood sugar is higher than normal but not high enough to be considered diabetes. Just 1 in 5 of those adults have been diagnosed.5 Without widespread screening and care that supports dietary and lifestyle changes, up to 70% of people with prediabetes will develop diabetes in their lifetime.6
Coverage enables early detection & treatment
Health care coverage – including private insurance, Medicaid, Medicare, and other health insurance – helps people access preventive care, including healthy living resources and screening. This supports early detection, timely medical interventions, and better health outcomes among people with diabetes.
 People with health insurance are far more likely to receive regular medical care, including preventive screenings and blood sugar checks that can help to identify risk factors and enable early detection. As a result, they are 55% less likely to have undiagnosed prediabetes or diabetes than people without health insurance.7
People with health insurance are far more likely to receive regular medical care, including preventive screenings and blood sugar checks that can help to identify risk factors and enable early detection. As a result, they are 55% less likely to have undiagnosed prediabetes or diabetes than people without health insurance.7
Coverage increases access to the regular care visits needed to develop treatment plans, monitor progress, and support patients in sustaining lifestyle that improve diabetes outcomes. Coverage also helps people access needed medications to control their blood sugar.
- Among people with diabetes, those with health insurance are 80% more likely to have had their blood sugar checked by a doctor in the past year.
- People with diabetes who have health insurance are also 56% more likely to have seen a diabetes specialist in the past 2 years.8
- People who have health insurance are 63% more likely to take important medications like insulin, which helps lower blood sugar and prevents long-term complications such as diabetic retinopathy, which leads to vision loss.
- Those with health insurance are 37% more likely to achieve safer blood sugar levels (A1c <9.0%).9 This reduces risk of problems like vision loss, kidney disease, and stroke.10
- Coverage also increases access to medication and supports that help people control their blood pressure. Blood pressure control is a critical measure of diabetes management because high blood pressure (or hypertension) increases the risk of stroke, kidney disease, and other complications among people with diabetes.
Coverage can also save lives. A study comparing states that mandated access to diabetes coverage to those that did not found that access to coverage was associated with a 4% reduction in mortality rates. The largest benefits were linked to access to supports like like glucose (blood sugar) monitoring equipment, diabetes self-management training, and medical nutrition therapy.11
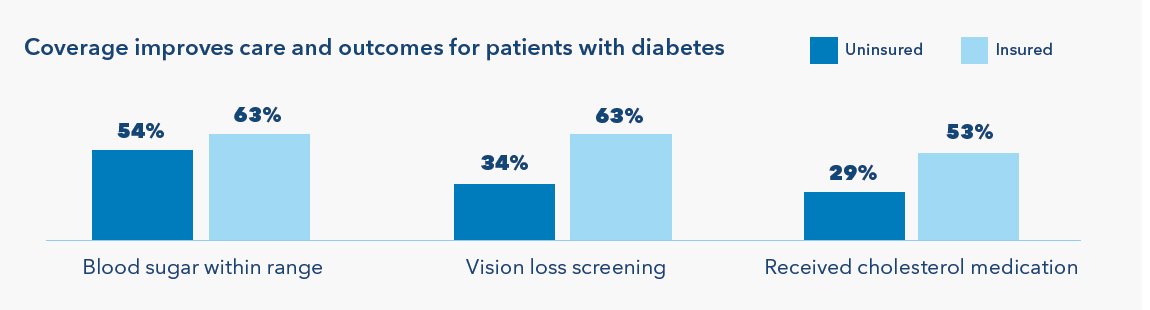
Data sources: NHANES 2017-2020 for uninsured & insured individuals ages 20-64; Blood sugar within range = A1c < 8%; Vision loss screening = Eyes dilated for retinal exam in last year; Received cholesterol medication = Received ≥1 courses of statins in the last year
The Kaiser Permanente approach
At Kaiser Permanente, we promote better outcomes for members with prediabetes and diabetes by investing in prevention, proactively screening for risk factors, and delivering evidence-based treatment. We help members enroll in programs that support healthy lifestyles, such as free and low-cost physical activity and nutrition counseling programs. Since unmet social needs – such as food insecurity, unstable housing, chronic stress, and limited transportation – can interfere with medication adherence, follow-up care, and healthy behaviors, our health care teams are trained to ask about health-related social needs and connect members with resources that help them access safe housing and healthy food.
Early detection is central to our approach. Kaiser Permanente offers the nationally recognized Diabetes Prevention Program, which has demonstrated lasting success in helping participants reduce diabetes risk and even reverse prediabetes. This cost-effective program combines personalized coaching, group support, and evidence-based lifestyle strategies to help members eat healthier, stay active, and maintain a healthy weight.12 Studies have shown that completing this type of program reduces the risk of developing diabetes by 58%. Even 10 years after completing the program, participants are still 34% less likely to develop diabetes.13
For members diagnosed with diabetes, Kaiser Permanente’s comprehensive diabetes programs deliver coordinated, evidence-based care tailored to individual needs. Every member is paired with a trained diabetes care manager who supports blood sugar monitoring, medication management, and communication across the care team, which includes physicians, health educators, and dietitians. Members also have access to diabetes education classes and ongoing coaching to help sustain healthy routines. As a result, 69% of our members with diabetes kept their blood sugar within healthy ranges and 87% had controlled blood pressure in 2024.14
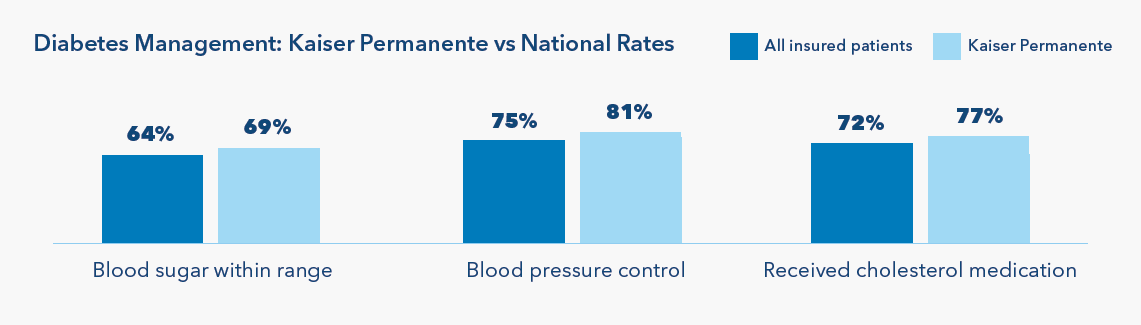
Health care coverage matters, and integrated care approaches are particularly effective at improving outcomes. Regular screenings and diabetes management programs support high-quality, evidence-based care, improving health outcomes and reducing both patients’ financial burdens and health care costs to the U.S. health system.
