
Integrated Care Stories
Cutting cancer risk through screening
Kaiser Permanente achieves better outcomes through a combination of care coordination, comprehensive data collection and use, and aligned incentives that all promote affordable, high-quality care. This case study, part of our Integrated Care Stories series, highlights the benefits of Kaiser Permanente’s approach.
The challenge
Cancer remains a leading cause of death in the United States and a significant driver of health care costs. In 2025, an estimated 2 million people will be diagnosed with cancer and 618,000 will have a cancer-related death.1 The incidence of cancer is increasing for many common cancers, including 6 of the top 10.2
Fortunately, some cancers—including breast, colorectal, prostate, and cervical cancer—can be identified through screening,3 and cancer detection and treatment has become increasingly effective. Over the past 3 decades, the cancer death rate has decreased by 33% nationally, thanks to smoking-cessation programs, earlier detection, and improved treatments.4
The integrated care and coverage solution
Kaiser Permanente’s integrated care approach enables us to identify risks and provide preventive care and treatment. We send our members personalized reminders about preventive care actions they can take to reduce their risks, and we alert both our members and our care teams about overdue cancer screenings. We also leverage new innovations to make screening easier, like providing at-home testing kits for colorectal cancer.
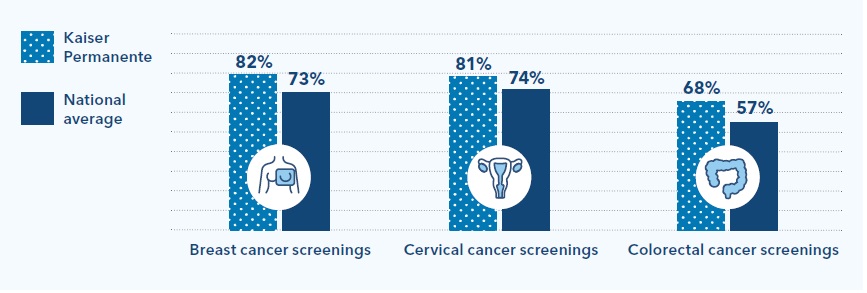
As a result, Kaiser Permanente has achieved higher screening rates than the national average for breast cancer (82% vs. 73%), cervical cancer (81% vs. 74%), and colorectal cancer (68% vs. 57%).6 This allows us to provide high-quality follow-up care early, when screening identifies potential health problems.
How Kaiser Permanente’s integrated care and coverage model supported this innovation
Integrated data for each member:
Members can easily access their personal data through Kaiser Permanente’s comprehensive, interconnected data system. They can see detailed health information, connect with their care team, and access telehealth services through kp.org, our secure, web-based member portal. With real-time access to electronic health records, Kaiser Permanente care teams review screening rates, identify individuals who may need additional support, and conduct personalized outreach.
For example, we are working to expand access to cervical cancer screenings through research and pilot programs testing at-home HPV kits. In select regions, eligible patients overdue for screening may receive a mailed kit, helping us evaluate new ways to deliver preventive care.
Connected, coordinated care teams:
Members benefit from well-coordinated care in the Kaiser Permanente system. Clinicians can easily coordinate with one another and seamlessly refer patients to other team members— primary care doctors, specialists, lab technicians, pharmacists, and other health care professionals. Our attention to coordinated screening helps us detect cancer earlier, improving treatment success rates and overall health outcomes. When cancer is identified, we provide timely and effective cancer treatment through multidisciplinary teams, including oncologists, radiologists, and care coordinators.
For example, one Kaiser Permanente member with a family history of cancer was referred by her physician to a Kaiser Permanente hereditary cancer program, which includes genetic counselors, breast surgeons, gynecologists, plastic surgeons, and therapists who can support the patient. She met with a genetic counselor to understand the screening process and make the decision to get screened. A genetic mutation was found, and her care team worked closely with her to design and follow through on a personalized early cancer detection plan, alternating mammograms and MRIs every 6 months. This approach detected early-stage breast cancer, and her care team provided early treatment, reducing the risk of recurrence to just 2%.
We provide timely and coordinated screening and treatment for cancers that can be detected early, including breast cancer, prostate cancer, colorectal cancer, and cervical cancer. As part of the National Cancer Institute’s Cancer Screening Research Network, Kaiser Permanente contributes to nationwide efforts to identify approaches that improve detection of cancers and promote treatment advances.
Flexibility within a budget:
The Kaiser Foundation Health Plan collects member premiums in advance and then pays delivery system partners for members’ care throughout the year. This creates the flexibility within and across the health plan, the hospitals, and the medical groups to deploy those resources to best meet our members’ needs and encourages wise use of resources.
Instead of relying on revenues generated when patients are sick, we are incentivized to invest in longer-term infrastructure and population health investments that improve long-term outcomes, and to provide timely, effective, and efficient care and service that allow us to retain and expand our membership.
Investing in screenings that detect cancer early improves outcomes and often reduces the need for costly treatments for more advanced cancer. This reduces financial burdens for individual patients, for health systems, and for the broader U.S. health system.
For example, in the first year of breast cancer treatment, the average cost of treating more localized breast cancer is $60,637 for stage 0 cancer or $82,121 for stage 1 or 2, while treatment costs are higher for later stage breast cancer ($129,387 for stage 3 and $134,682 for stage 4).7
Experts estimate that earlier cancer detection could save the U.S. health care system an estimated $26 billion annually.8
Kaiser Permanente’s value-based, integrated care and coverage model differs from much of the United States health care system, which relies on disconnected clinical practices paid through fee-for-service. These disconnected approaches typically result in highly fragmented care, a focus on quantity of services with less focus on ensuring high-quality care, and an emphasis on acute care rather than long-term investments in population and community health.
Kaiser Permanente achieves better outcomes through a combination of care coordination, comprehensive data collection and use, and aligned incentives that all promote affordable, high-quality care. This case study, part of our Integrated Care Stories series, highlights the benefits of Kaiser Permanente’s approach.
References
- Siegel RL, Kratzer TB, Giaquinto AN, Sung H, Jemal A. Cancer statistics, 2025. CA Cancer J Clin. 2025 Jan-Feb;75(1):10-45. doi: 10.3322/caac.21871. Epub 2025 Jan 16. PMID: 39817679; PMCID: PMC11745215.
- American Cancer Society. (2025). Cancer facts & figures 2025. Atlanta, GA: American Cancer Society.
- American Cancer Society. (2025). Cancer facts & figures 2025. Atlanta, GA: American Cancer Society.
- National Cancer Institute, Surveillance, Epidemiology, and End Results Program (SEER). (n.d.). Cancer stat facts: Cancer of any site. Retrieved from https://seer.cancer.gov/statfacts/html/all.html, Zafar, S. Y., & Abernethy, A. P. (2013). Financial toxicity, Part I: A new name for a growing problem. Oncology, 27(2), 80–81, 149. https://pubmed.ncbi.nlm.nih.gov/23530397/
- National Cancer Institute, Surveillance, Epidemiology, and End Results Program (SEER). (n.d.). Cancer stat facts: Cancer of any site. Retrieved from https://seer.cancer.gov/statfacts/html/all.html, Zafar, S. Y., & Abernethy, A. P. (2013). Financial toxicity, Part I: A new name for a growing problem. Oncology, 27(2), 80–81, 149. https://pubmed.ncbi.nlm.nih.gov/23530397/; Hall JM, Mkuu RS, Cho HD, Woodard JN, Kaye FJ, Bian J, Shenkman EA, Guo Y. Disparities Contributing to Late-Stage Diagnosis of Lung, Colorectal, Breast, and Cervical Cancers: Rural and Urban Poverty in Florida. Cancers (Basel). 2023 Oct 31;15(21):5226. doi: 10.3390/cancers15215226. PMID: 37958400; PMCID: PMC10647213; Brill, J. V. (2020, November 16). Screening for cancer: The economic, medical, and psychosocial issues. The American Journal of Managed Care. https://www.ajmc.com/view/screening-for-cancer-the-economic-medical-and-psychosocial-issues
- Kaiser Permanente, Value-Based Care Designed to Deliver Maximum Cost Savings, https://business.kaiserpermanente.org/california/care-value/managing-costs (cites 2023 KP HEDIS data); and Sabatino SA, Thompson TD, White MC, Villarroel MA, Shapiro JA, Croswell JM, Richardson LC. Up-to-Date Breast, Cervical, and Colorectal Cancer Screening Test Use in the United States, 2021. Prev Chronic Dis. 2023 Oct 26;20:E94. doi: 10.5888/pcd20.230071. PMID: 37884318; PMCID: PMC10625435.
- Blumen H, Fitch K, Polkus V. Comparison of Treatment Costs for Breast Cancer, by Tumor Stage and Type of Service. Am Health Drug Benefits. 2016 Feb;9(1):23-32. PMID: 27066193; PMCID: PMC4822976.
- Brill, J. V. (2020, November 16). Screening for cancer: The economic, medical, and psychosocial issues. The American Journal of Managed Care. https://www.ajmc.com/view/screening-for-cancer-the-economic-medical-and-psychosocial-issues; Kakushadze, Z., Rhaghubanshi, R., and Yu, W. Estimating cost savings from early cancer diagnosis (2017). Data 2(3), 30. https://doi.org/10.3390/data2030030