
Integrated Care Stories
Meeting patients’ needs through telehealth
Kaiser Permanente achieves better outcomes through a combination of care coordination, comprehensive data collection and use, and aligned incentives that all promote affordable, high-quality care. This case study, part of our Integrated Care Stories series, highlights the benefits of Kaiser Permanente’s approach.
The challenge
During the COVID-19 pandemic, people needed telehealth services to get care while staying safe at home. Health care systems rushed to create new telehealth services or expand their virtual offerings. Many had not made the necessary investments in telehealth infrastructure before the pandemic. They faced multiple barriers, including high startup costs, lack of equipment, lack of physician buy-in, workflow challenges, and patient difficulties using the new or expanded telehealth technology.1
The integrated care and coverage solution
Kaiser Permanente was investing in and using telehealth long before the pandemic. For decades, health information technology has been a key feature of our integrated care delivery approach, as we capture and store information to track the full range of our members’ health conditions, test results, and treatments and use that information to improve their health. Kaiser Permanente’s experience managing large numbers of electronic health records has allowed us to build and improve a wide range of telehealth offerings over many years.
With a strong telehealth infrastructure already in place, Kaiser Permanente was able to rapidly scale our virtual services to meet increased demand during the pandemic.2
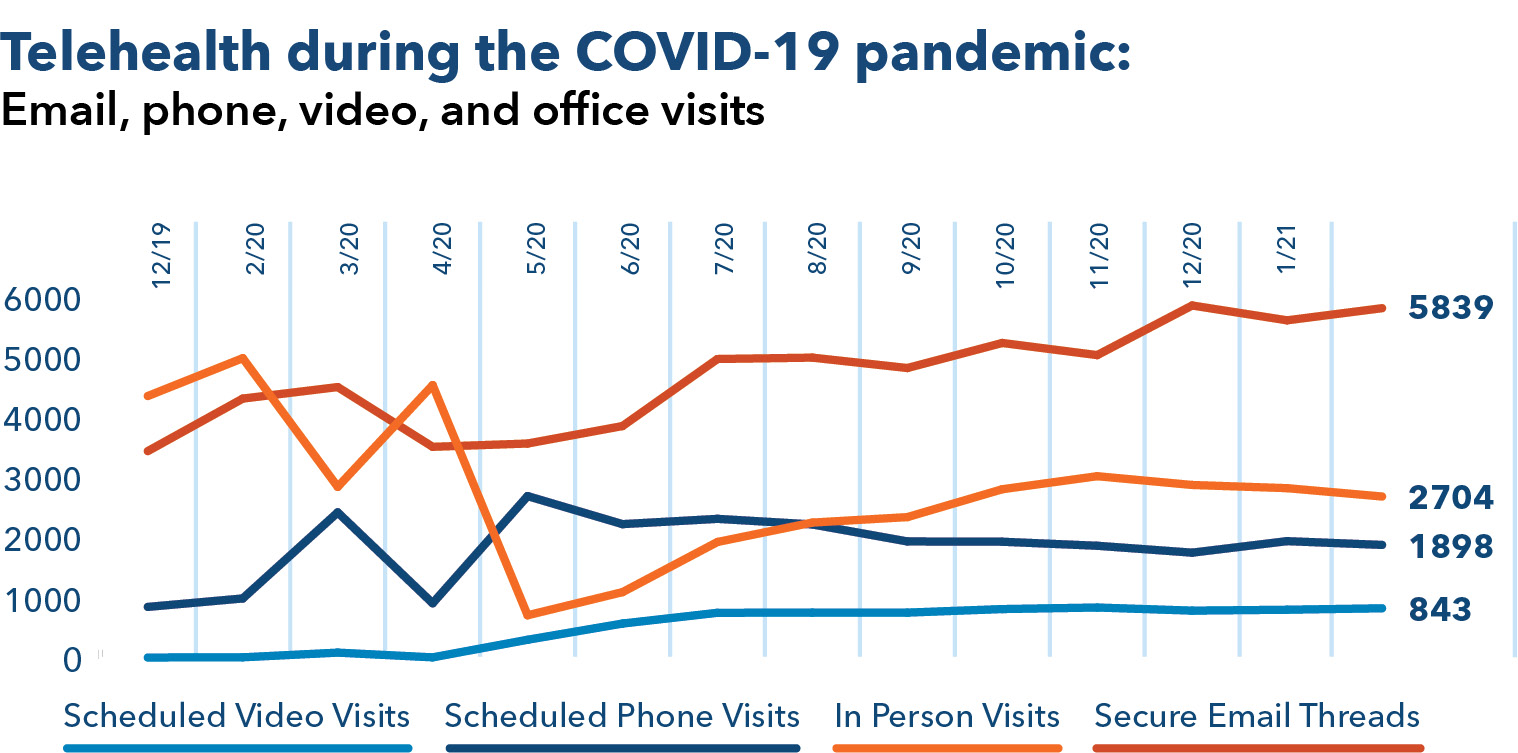
Telehealth use increased quickly in early 2020 and has remained high compared to rates before the pandemic, even as in-person care has resumed. Members have been satisfied with telehealth, with 8 out of 10 members saying they plan to continue using telehealth services after the pandemic.3
Building on these successes, we continue to evolve and innovate. Kaiser Permanente has begun piloting the use of mental health and wellness mobile apps, a particularly important offering as the pandemic upended routines and added new stresses to people’s lives. Clinicians can refer members to 3 mindfulness and meditation apps designed to reduce anxiety and improve sleep, and 3 cognitive behavioral therapy apps that provide interactive support activities and coaching. Care teams are tracking app use to assess their value and make improvements.4 Other recent innovations include digital-first insurance options, which leverage our telehealth capabilities to provide a new alternative for affordable coverage. Through these plans, members access their care team through telehealth services first, but can come in for in-person office visits as well.5 Kaiser Permanente also is helping a network of safety net organizations find new approaches to expand virtual care access for populations experiencing homelessness and others with access challenges.6
How Kaiser Permanente’s integrated care and coverage model supported this innovation
Connected, coordinated care teams
Members benefit from well-coordinated care in the Kaiser Permanente system. Clinicians can easily coordinate with one another and seamlessly refer patients to other team members — primary care doctors, specialists, lab technicians, pharmacists, and other health care professionals.
All Kaiser Permanente care encounters — in-person or virtual — are directly connected to members’ electronic health records and are accessible to their entire health care teams. More than half of our members who use telehealth services during the COVID-19 pandemic said their health concerns were resolved after their virtual visit. When additional support was needed, members could see their doctors in person in our clinics.
Flexibility within a budget
The Kaiser Foundation Health Plan collects member premiums in advance and then pays delivery system partners for members’ care throughout the year. This creates the flexibility within and across the health plan, the hospitals, and the medical groups to deploy those resources to best meet our members’ needs. Instead of relying on revenues generated when patients are sick, we are incentivized to invest in longer-term infrastructure and population health investments that improve long-term outcomes, and to provide timely, effective, and efficient care and service.
Kaiser Permanente began using electronic health records in the 1960s, and we invested in connecting electronic health records across our full network more than a decade ago.7 Thanks to this investment, we developed our telehealth capabilities early, which, in turn, allowed us to scale our offerings quickly during the pandemic. We continue to create new telehealth care and coverage options.
Integrated data for each member
Members can easily access their personal data through Kaiser Permanente’s comprehensive, interconnected data system. They can see detailed health information, connect with their care team, and access telehealth services through kp.org, our secure, web-based member portal.
In 2004, Kaiser Permanente launched our integrated, secure electronic health records system, which connects information for all our members across all our medical offices and hospitals.8 Linked to this system, we use the secure kp.org portal to make it easy for members to access their personal records and track and manage their health. Members can view their medical history, schedule appointments, view test results, order prescription drugs, view health and wellness resources, and access telehealth services.
Information sharing across clinical care teams
Clinicians have access to all Kaiser Permanente medical data for every member, enabling care teams to identify opportunities to improve the safety and quality of care. Kaiser Permanente tracks and maintains records over decades, enabling a long-term perspective on each individual’s health over time. Our care teams also can make well- informed decisions based on a full range of patient information and can easily connect with each other to work effectively as a team.
Doctors can leverage telehealth tools to consult with other care team members by phone, video, and sometimes secure text messaging as well. For example, a primary care doctor may connect with a specialist to access additional expertise quickly and ensure high-quality care.
Focus on individual and population health
Our mission, and our long-term perspective, motivates us to address individual and community drivers of health. We work to eliminate racial and economic disparities, make community investments, and collaborate with community partners. These investments in individual and population health help us retain our members, and Kaiser Permanente benefits when those long-tenured members and the broader communities we serve realize positive health outcomes.
Kaiser Permanente is investing in equitable telehealth access for our members by providing telehealth care in more than 150 languages and offering access to audio-only services for members who prefer or need this option.9 We also distributed over $5.25 million to safety net organizations working to expand telehealth access during the pandemic. These investments and innovations will help expand long-term telehealth access.
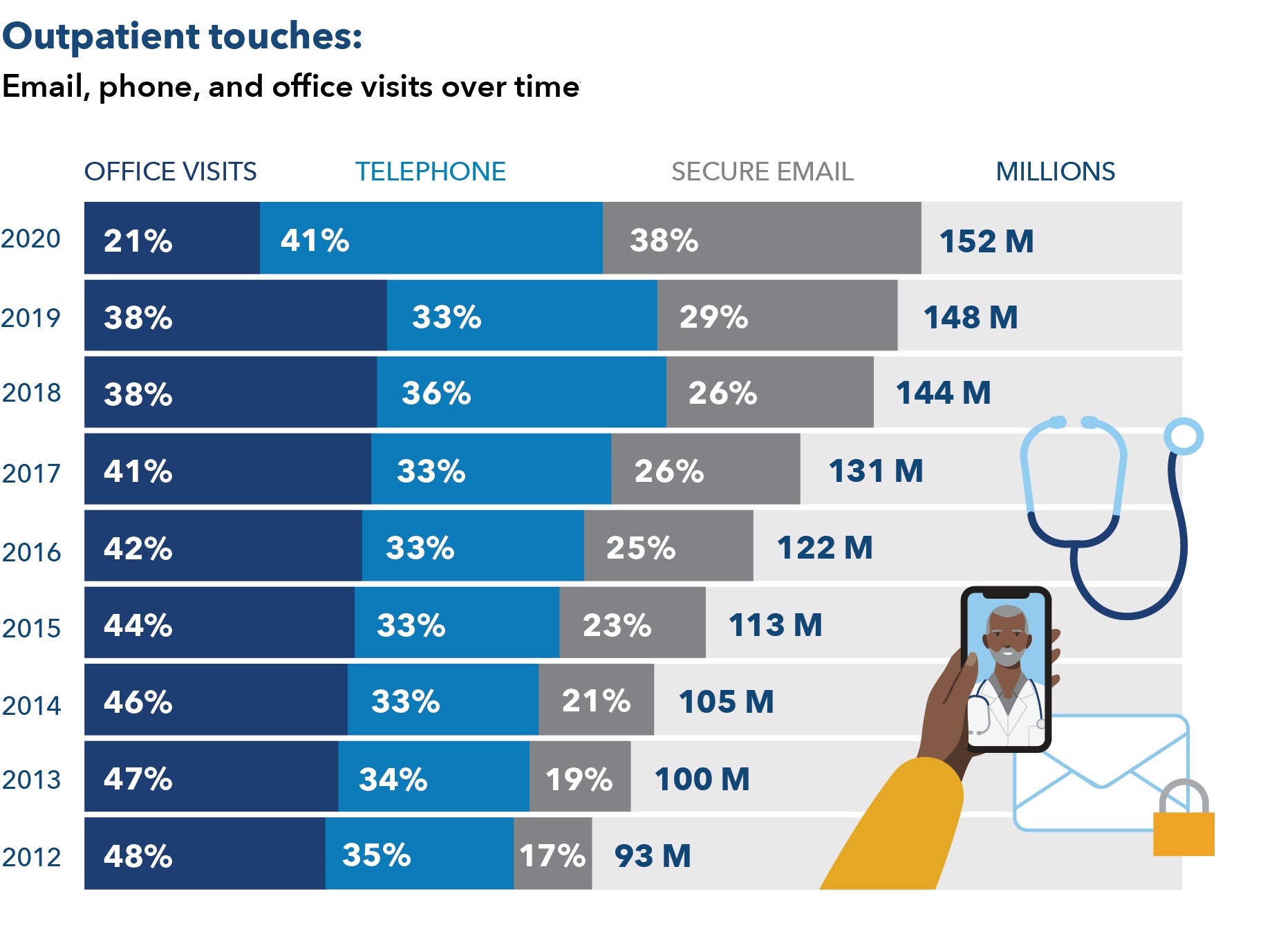
Kaiser Permanente’s integrated care and coverage model differs from much of the United States health care system, which relies on disconnected clinical practices paid through fee-for-service. These disconnected approaches typically result in highly fragmented care, a focus on quantity of services rather than high-quality care, and an emphasis on acute care rather than long-term investments in population and community health.
Kaiser Permanente achieves better outcomes through a combination of care coordination, comprehensive data collection and use, and aligned incentives that all promote affordable, high-quality care. This case study, part of our Integrated Care Stories series, highlights the benefits of Kaiser Permanente’s approach.
Promoting digital equity
Digital technologies are evolving rapidly – shaping new health care approaches, and changing the way we access education, jobs, and other critical resources.
Telehealth after the pandemic: perils, promise, and possibility
Telehealth gives us a glimpse into our health care future – but public and private sector choices will determine whether telehealth fully lives up to its promise.
Telehealth during the pandemic: Kaiser Permanente’s experience
In 2020, the COVID-19 pandemic forced many people to stay at home to reduce potential transmission. In health systems that had already deeply invested in building and using telehealth capacities, including Kaiser Permanente, telehealth use increased.
Lawmakers must act to boost telehealth and digital equity
Making key pandemic-era telehealth policies permanent and ensuring more people have reliable internet access will improve health outcomes for all.
1 C. Lieneck, et al. “Rapid Telehealth Implementation during the COVID-19 Global Pandemic: A Rapid Review,” Healthcare, 8(4), 517, November 29, 2020, https://doi.org/10.3390/healthcare8040517.
2 Kaiser Permanente Institute for Health Policy, “Telehealth During the COVID-19 Pandemic: Kaiser Permanente’s Experience,” June 17, 2021, https://www.kpihp.org/blog/telehealth-during-covid-booklet/kaiser-telehealth-during-covid-19/.
3 Kaiser Permanente National Market Research, June 2020 Member COVID-19 Survey
4 D. Mordecai, et al. “How Kaiser Permanente Created a Mental Health and Wellness Digital Ecosystem,” NEJM Catalyst Innovations in Care Delivery, January 2021, https://doi.org/10.1056/CAT.20.0295; and Kaiser Permanente, “Just What the Doctor Ordered: Mental Health and Wellness Apps,” Kaiser Permanente Press Release, December 16, 2020. https://about.kaiserpermanente.org/our-story/news/announcements/just-what-the-doctor-ordered-mental-health-and-wellness-apps.
5 Kat Jercich, “Kaiser Permanente Launches “Virtual-First” Health Plan in Washington,” Health Care IT News, September 14, 2020, https://www.healthcareitnews.com/news/kaiser-permanente-launches-virtual-first-health-plan-washington; Kaiser Permanente Business, “Virtual Complete Plans,” https://business.kaiserpermanente.org/health-plan/virtual-complete Sept. 21, 2021; and Kaiser Permanente, “Seamless Care Becomes a Virtual Reality,” https://virtualforward-midatlantic.kaiserpermanente.org/, Sept. 21, 2021; Kaiser Permanente, “Value Plan,” https://healthy.kaiserpermanente.org/shop-plans/virtual-plan, Sept. 21, 2021.
6 Kaiser Permanente, “Supporting access to telehealth for vulnerable populations,” https://mykp.kp.org/en/news/national/supporting-access-to-telehealth-for-vulnerable-populations.html, May 24, 2021.
7 Kaiser Permanente, “Decades of Health Records Fuel Kaiser Permanente Research,” About Kaiser Permanente, https://about.kaiserpermanente.org/our-story/our-history/decades-of-health-records-fuel-kaiser-permanente-research March 6, 2013; Health IT Outcomes, “Kaiser Permanente Completes Electronic Health Record Implementation,” March 5, 2010, https://www.healthitoutcomes.com/doc/kaiser-permanente-completes-electronic-health-0001; Catherine Chen, et al., “The Kaiser Permanente Electronic Health Record: Transforming and Streamlining Modalities of Care,” Health Affairs, March 2009, https://www.researchgate.net/publication/24191168_The_Kaiser_Permanente_Electronic_Health_Record_Transforming_And_Streamlining_Modalities_Of_Care; and Benjamin Wheatley, “Transforming Care Delivery through Health Information Technology,” The Permanente Journal, Winter 2013, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3627785/.
8 Kaiser Permanente International, “Kaiser Permanente: The Electronic Health Record Journey,” https://international.kaiserpermanente.org/resources/ehr_journey/, July 2019; and Health IT Outcomes, “Kaiser Permanente Completes Electronic Health Record Implementation,” March 5, 2010, https://www.healthitoutcomes.com/doc/kaiser-permanente-completes-electronic-health-0001.
9 Kaiser Permanente Institute for Health Policy, “Telehealth During the COVID-19 Pandemic: Kaiser Permanente’s Experience,” June 17, 2021, https://www.kpihp.org/blog/telehealth-during-covid-booklet/kaiser-telehealth-during-covid-19/